 The supermarket shelves are lined with products encouraging us to keep our lady parts clean and pleasant-smelling . Many of us still remember the line “Do you ever get that not-so-fresh feeling?” from a douche commercial years ago that made many a woman begin doubting their vaginal cleanliness at a very young age. The truth is that most women’s natural scent is normal. Your vagina doesn’t need to smell like that field of flowers on the box of feminine deodorant spray. Why does the vagina smell? The vagina is a carefully balanced ecosystem of fluid (discharge) and bacteria meant to keep the vaginal PH at a healthy 4.5. This combination of fluid and bacteria that make up the vaginal discharge that can, at times, emit certain odors. Most of these odors are natural and normal, but there are times when excess odor can signal a problem. So what is a “normal” amount of odor? After performing a very unscientific poll of all the gynecologist I know, we determined that one can smell a normal vagina from 1 foot away. More pungent odor or any associated with pain, burning or itching should prompt a visit to your provider. Some common causes of vaginal odor include: Bacterial Vaginosis (BV) – The vagina is normally colonized with healthy bacteria, but if something disturbs the ecosystem, then unhealthy bacteria like BV can take over. BV is most commonly caused by an overgrowth of the bacteria Gardnerella vaginalis. Symptoms include a thin grey, runny discharge and a strong fishy odor. The odor is more pungent when in contact with semen, so often women will first notice this as a strong odor after sex. BV is annoying and can increase your risk of other infections, but is easily treated with antibiotics. Your Diet – The old adage “You are what eat” is true, all the way down to your lady bits. Garlic, onion, asparagus, and curry are few of the more odoriferous foods known to affect body odor. Medications/ Supplements - Medications such as antibiotics can affect the bacterial balance of your vagina leading to changes in odor and discharge. Antihistamines can lead to vaginal dryness and decreased vaginal secretions, which can also have an effect. Additionally, herbal therapies and the newly popular essential oils can lead to changes in vaginal odor. Sweat - Much like your underarms, the skin around your genitals is prone to excessive sweating. Sweat when combined with discharge can escalate the natural musk to a whole new level of stank. This is a natural odor, though sometimes slightly unpleasant. To minimize the smell, change clothes after exercising and wear breathable fabrics. Hormonal Changes – The amount of discharge varies throughout menstrual cycles. Hormonal therapies, birth control pills and vaginal creams can have an effect the vaginal PH and odor as well. Menopause also leads to major changes as the decreasing estrogen levels can lead to increasing incidence of yeast infection and BV. A Forgotten Tampon – There is one odor that is so foul, it is unlike anything you have every smelled in your entire life. It’s the one smell that makes even the gynecologist gag: the forgotten tampon. The patients on many occasions have described the odors as ”it smells like something crawled up in there and died.” I would have to agree that this is an honest statement. While the odor is particularly offensive, it does resolve quickly after the tampon is removed. Rarely, the retained tampon can also lead to serious infection, so it is important to see your doctor should this occur (symptoms include a brown discharge and odor). Douching is never indicated for vaginal odor or any other reason. It only further changes the bacterial content and can spread infection. You do not need to insert anything inside your vagina to clean it: no douche, no essential oils, no soap, no Listerine (yes, these are all things I’ve had patients use to ‘clean themselves’). Simply think of the vagina as a “self-cleaning oven.” If you’re concerned about your odor, but have no other symptoms, you may first try increasing your water intake and cutting out any odorous foods. You might also take a probiotics to help restore normal bacterial balance. For proper hygiene, clean the external area of your vagina (vulva and labia) with a mild soap. If odor persists despite these measures, then follow up with your provider. By Heather Rupe, DO http://blogs.webmd.com/womens-health/2014/10/why-does-my-vagina-smell.html
0 Comments
Although breast self-exams can be life-saving, doing them every month is just one more time consuming, anxiety-provoking task on your to-do list.
Feel for lumps in the shower, then stand in front of the mirror, then lie down and feel again. Use this kind of motion, that type of pressure. Repeat every month. Kudos to you if you are making the time, but if you’re only doing them occasionally, that’s ok too. “The very rigid and structured monthly breast self-exam that you take very seriously, has kind of gone by the wayside,” said Dr. Alyssa Dweck, a board-certified obstetrician and gynecologist and co-author of “V is for Vagina.” Although major health organizations previously recommended women do breast self-exams every month without fail, studies show they don’t improve survival odds and may even increase the amount of unnecessary biopsies. Experts agree breast self-exams are a good idea but it’s more important to know what your breasts look and feel like rather than worrying too much about what method to use. “We think it’s important for women to know what’s normal for them so they would recognize a change if a change occurred,” said Susan Brown, a registered nurse and managing director of health and mission program education at Susan G. Komen. So regardless of when and how often you do a breast self-exam, here are some tips: • Do the breast self-exam when your period ends so your breasts are less likely to be tender or swollen. • Stand in front of the mirror and raise your arms above your head, then lower them at your sides. Look for any differences in your breasts. • Use the pads of your fingers to feel for lumps, bumps and tender spots. You can do it in the shower, sitting or lying down. • Use an up and down, circular or wedge (start at the outer edge of the breast and move towards the nipple and back again) motion. It doesn’t matter which one you use but do the same one each time so you know what’s normal. • Feel under your armpits for enlarged lymph nodes. Here are some changes to look for and talk to your doctor about: • Nipples that retract or are pulled in. For some women, this is normal and no reason to worry. • A lump, hard knot, or thickening in the breast or the underarm. • Dimpling or puckering of the skin anywhere in the breast. • An unusual rash or a rash that looks like an orange peel. • A sudden change in the size or shape of the breasts. It’s normal for breasts to be asymmetrical. • A clear or milky discharge from the nipple (other than breast milk). It’s not usually a sign of cancer and might be a sign of an elevated level of the hormone prolactin. Nevertheless, tell your doctor. • Spontaneous grey, black, dark green or bloody nipple discharge. • Swelling, warmth, redness, or darkening of the skin. • An itchy, scaly sore or rash on the nipple. • New pain in one spot of the breast that doesn’t subside. by Julie Revelant is a freelance writer and copywriter specializing in parenting, health, healthcare, nutrition, food and women's issues. 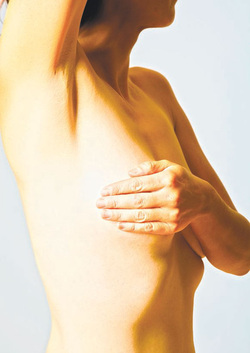 Individuals diagnosed with some form of cancer often ask themselves and their physicians, “Could I have done something to prevent this?” Women who are concerned about breast cancer also may wonder if they can prevent this potentially deadly disease, wondering if there is a pill, a vitamin, or another method to keeping the cancer at bay. Unfortunately, there is no guaranteed way to prevent breast cancer. However, there are many different steps to take that may help reduce the risk for cancer or increase the odds that if breast cancer is present, it can be found at a more treatable stage. There is no exact cause of breast cancer, but many experts agree that certain lifestyle choices as well as genetics can increase an individual’s risk. A woman’s risk also increases as she ages. When a woman is in her 30s, her risk of developing breast cancer is roughly four out of 1,000. By the time she reaches her 60s, that risk has increased to 37 out of 1,000. Though women can’t reverse the aging process, they can gain a greater understanding of additional risk factors for breast cancer and follow medical guidelines concerning breast cancer screenings. Here are some things to know: Family history: Having a sister, mother, daughter, or two or more close relatives with a history of breast cancer increases a woman’s risk, particularly if these diagnoses were made when the relatives were under the age of 50. Such women should begin testing for breast cancer at an early age. Personal history: If you’ve already experienced cancer in one breast or another part of your body, you are at an increased risk of getting cancer again. Breast cancer can turn up in the other breast or even in the same breast as before. Inheritance of genetic mutations: Individuals with mutations in the BRCA1 and BRCA2 genes are much more likely to get breast cancer, says the National Cancer Institute. The risk also increases for colon or ovarian cancer. In normal cells, BRCA1 and BRCA2 help ensure the stability of the cell’s genetic material and help prevent uncontrolled cell growth. Mutation of these genes has been linked to the development of hereditary breast and ovarian cancer. A simple blood test and a genetic work-up can point out mutations in these important genes. Race: Although Caucasian women are more likely to get breast cancer than black, Hispanic, or Asian women, black women typically are more susceptible to an aggressive type of breast cancer called basal-like tumor. Limited access to healthcare can also increase the risk of cancer fatality regardless of race. Childbearing age: Women who first gave birth after age 30 have a greater chance of developing breast cancer than women who had children before reaching 30 years of age. Women who have never had children are also at a higher risk. Women who breastfeed lower their risk for breast cancer. Hormones: Women with a longer span of “high-estrogen years” are more at risk for breast cancer. This includes women who had their first menstrual cycle prior to age 12 and women who still were experiencing menopause after age 55. Anyone undergoing hormone-replacement therapy or participating in estrogen-raising therapies also has a higher risk of developing breast cancer. While many of these factors are out of your control, there are other risk factors that you can control: Alcohol consumption: Avoiding or limiting alcohol consumption can lower your risk for breast cancer. Drinking alcohol has been traced to higher estrogen levels in the body. Obesity: Being overweight can also increase risk of developing breast cancer. Inactivity: Failure to exercise can increase your risk. That’s because regular exercise and a healthy diet contribute to the body’s defense system, ensuring it is more capable of fending off disease. Tobacco products: Use of cigarettes, cigars, or chewing tobacco increases your risk for many different cancers. Infrequent doctor visits: Routine physical check-ups by a general doctor or one who specializes in women’s health can make the difference between an early breast cancer diagnosis, for which treatment is highly successful, or late-stage diagnosis, which is not as easily treated. Those who do not go for screenings put themselves at an elevated risk. Breast cancer cannot be prevented, but there are many methods to reducing risk factors associated with the disease. Article from : http://www.downtownexpress.com/2014/10/03/breast-cancer-risk-factors/  With the cesarean section (C-section) rate in the U.S. approaching a staggering 32%, more women are faced with the often difficult decision of whether or not to attempt a vaginal delivery after C-section (VBAC). Of women who attempt VBAC, 30% will end up with another C-section during labor. The 70% of women who have a successful VBAC experience a quicker, less painful recovery and a lower complication rate for baby and mom. But there are risks of complications with VBAC, too. They are rare, but when they do happen they can be extreme. When a woman has a C-section, a cut is made in the lower part of her uterus to pull out the baby. The doctor then sews the uterine incision neatly back together, but it is always a bit weaker. With her next pregnancy, if a vaginal delivery is attempted, the pressure of labor contractions can cause the old uterine scar to break open 1% of the time. If this rare uterine rupture does happen, the mom risks hemorrhage and loss of her uterus. In extremely rare cases, oxygen can be cut off to the baby, leading to brain damage or death. If you have had one to two C-sections, ask yourself these questions as you consider your next delivery. How many kids do I want to have? A scheduled repeat C-section carries its own risks, including bladder injury, infection, and increased rates of NICU admission for the baby. A C-section is a major surgery, and the more of them you have, the higher your chances of complications. The complications related to a fourth C-section are somewhat higher than the third, and a fifth C-section carries extremely high risk. A pregnancy after four C-sections has a 10% chance of the placenta growing into the uterus (a condition called accreta), which is dangerous and usually results in a preterm delivery and a hysterectomy. If you’re thinking about having more than three children, you should strongly consider a VBAC. How important is a vaginal delivery to me? All births are beautiful miracles, but a VBAC delivery is almost triumphant. As the woman delivers, she finally gets to experience the birth that has been two pregnancies in the making. A lot of women have a strong desire to have a vaginal delivery. They feel this is an important life experience, and for them a 1% risk may seem worth it — others not so much. Have I had other vaginal deliveries? If you’ve had other vaginal deliveries before your C-section, your chance of successful VBAC is higher. Your risk of rupture is still there, but your chance for successful vaginal delivery is around 90%. Why did I have my first C-section? Is the reason for your first C-section something that can be changed? Was your first baby a breech 11-pounder, and this one is normal-sized and head down? If so, you might be a good candidate for VBAC. But if you were carrying a normal-sized baby last time, and you went into spontaneous labor and were unable to deliver vaginally, then it’s likely that the same thing could happen again. So, perhaps a repeat C-section might be a better option. There’s no “magic 8 ball of labor” that will tell us for sure if your VBAC will be successful. But if the reason for your first C-section is not present this time, than a vaginal delivery is more likely to be successful. Do my provider and hospital offer VBAC? If you plan to try for a VBAC, you need to make sure your hospital is equipped and your provider is on board. In order to improve the safety of VBACs, hospitals have to be ready at a moment’s notice to do an emergency C-section in case the uterus breaks. When a break happens, the placenta usually becomes detached from the uterus, meaning no oxygen for the baby. The obstetrician must get the baby out very quickly to prevent brain damage from lack of oxygen. If you live in a more rural area, you may need to travel to a more urban hospital in order to get a VBAC. In the end, each woman’s unique pregnancy history will determine whether VBAC is the right option for her. If you’re done having children with two, the chance of an easier recovery may not be worth the risk of rupture. But if you had a terrible experience with your first C-section and have a strong desire to experience natural child birth or want a larger family, then a 1% risk may seem minimal to you. Talk to your provider about your overall chance of a successful VBAC as you carefully weigh the risks and benefits. By Heather Rupe, DO  Data released by the Department of Health in 2013 cited that 25 percent of Filipino adults, or about 14 million, suffer from hypertension (high blood pressure), a major risk factor for heart disease and stroke. Heart disease and stroke remain two of the top killers of Filipinos and comprise 35 percent of total deaths. Philippine Health Statistics data show that in 2009 about 167,000 Filipinos died from heart disease and stroke. Half of these deaths were likely related to high blood pressure. An analysis done by the Philippine Institute for Development Studies (PIDS) further reveals that 34 percent of all cardiovascular deaths are happening prematurely or at ages below 60. Means of prevention Though the statistical realities of hypertension, stroke and heart disease have been divulged at length, little has been actually discussed on diet as a means of prevention, much less the potentials of a mineral such as potassium in significantly reducing the risk of stroke. A recent Physicians Committee for Responsible Medicine’s Sept. 5 Breaking Medical News noted that a diet rich in potassium reduces the risk of stroke for postmenopausal women. It shared a study published online in the American Heart Association journal Stroke. Reduction in risk PCRM noted that researchers analyzed the potassium intake of 90,137 postmenopausal women as part of the Women’s Health Initiative Observational Study. Women who consumed the most potassium reduced their risk of all stroke types by 12 percent and lowered their risk of ischemic stroke (stroke due to clot formation) by 16 percent, compared with those who consumed the least amount. FRUITS are also good sources of calcium, among other nutrients. Photo by Tessa R. Salazar PCRM noted that “the reduction in risk was even greater among women who had normal blood pressure, compared with those who had high blood pressure. High potassium intake was also associated with a reduced risk from death by all causes, compared with the lowest intake, during the 11 years of follow up.” “This study suggests that all women should consume more potassium from foods like sweet potatoes, bananas and white beans to meet or exceed daily recommendations,” it said. Like PCRM, preventive healthcare expert Neil Nedley, MD, has long advocated for vegan food (devoid of all forms of animal products, including dairy products) and high potassium foods to help reduce blood pressure. Nedley said: “There are many foods that can be freely eaten without concern about their sodium content,” he said in his book “Proof Positive,” where he cited food groups low in sodium such as fresh fruits, grains and cereals, unsalted nuts, vegetables and shredded wheat. Double benefit “Fruits provide a double benefit in that they are also high in potassium, which tends to reduce blood pressure even further. This is partially why a natural diet high in fruits, vegetables and grains is the answer to the blood pressure problem,” Nedley said, adding that, however, “any food that is low in sodium can be made high by shaking the salt dispenser over it.” Foods high in calcium content can also significantly lower blood pressure. Green leafy vegetables are good sources of calcium. A report on the research at the American Heart Association in 1992 warned against taking large amounts of calcium supplements. “Instead,” said Prof. James Dwyer who reported on that research, “people should get calcium through their diets … green leafy vegetables are good sources of calcium.” A common breakfast food, oatmeal, has been found to reduce blood pressure. In one study, 850 people were categorized for the amount of oatmeal they consumed. One bowl per day consumers had lower blood pressure and lower cholesterol. Managing blood pressure Nedley suggested the following for people who would want to manage their blood pressure: • Avoid low fiber foods such as meat (pork, beef, chicken and other livestock products) and dairy products (cow’s milk, cheese). • Eat plenty of fruits, vegetables, grains and unsalted nuts in moderation, and other low-sodium foods. • Avoid foods such as dill pickles, cured ham, Chinese rice, bouillon and other high-sodium foods. Read the labels. • Eliminate coffee, cola drinks and alcohol from the diet. • Stop smoking. • Give the salt shaker a rest. • Bring your weight down to the recommended level for your height and build. • Adopt an aerobic exercise routine, such as brisk walking. • Learn to cope with stress. By Tessa R. Salazar  (NAPSI)—Ovarian cancer, the eighth most commonly diagnosed and the fifth most common cause of cancer death for women in the UnitedStates, is sometimes called a “silent killer.” There is currently no reliable screening method to detect ovarian cancer and symptoms often go unnoticed. Early stages of ovarian cancer often present symptoms that are more commonly caused by other less serious conditions, such as abdominal pain, swelling or bloating, or pelvic pressure. As a result of late diagnosis, 75 percent of patients have ovarian cancer that has spread to nearby organs. The five-year survival rate for these ovarian cancer patients is less than 50 percent. “It is vitally important for women to understand that their risk of developing ovarian cancer and subsequent prognosis is influenced by several factors, including age, environmental and lifestyle factors, early stage of diagnosis, and family history,” said Sue Friedman, founder and Executive Director of Facing Our Risk of Cancer Empowered. “Additionally, the risk of developing ovarian cancer is increased in women with specific inherited genetic abnormalities. One of these risks is associated with BRCA 1 and BRCA 2 mutations.” Consider these facts and work with your doctor to understand your options for ovarian cancer treatment. Ovarian cancer facts and figures: • Approximately 22,000 U.S. women will be diagnosed with ovarian cancer in 2014. • Ovarian cancer is a disease in which cells in the ovaries grow out of control and form tumors, which are abnormal tissues that serve no function. • All women are at risk for ovarian cancer; however, roughly 90 percent of women who are diagnosed with ovarian cancer are older than 40. • The greatest number of ovarian cancers occur in women aged 60 years or older. • High-grade serous cancer is the most common and aggressive form of ovarian cancer. • Approximately 60-80 percent of ovarian cancer is of the serous subtype and as many as 95 percent of advanced ovarian cancers are of the serous subtype. • BRCA gene mutations can play a key role in serous ovarian cancer. In the general population, 1.4 percent of women will be diagnosed with ovarian cancer, while up to 40 percent of women with BRCA ½ mutations will be diagnosed with ovarian cancer in their lifetime. If you are living with ovarian cancer, be sure to talk to your doctor about all of your treatment options. And if someone you know has ovarian cancer or may be at risk, please visit www.myOCjourney.com, which is sponsored by AstraZeneca and designed to provide the support you need to live your best life as you fight ovarian cancer. this article comes from AstraZeneca You've probably seen the videos or at least heard the stories of women a month or two away from delivery and still pumping iron and running marathons. These pregnant phenoms elicit as much admiration as they do concern from onlookers.
If you're a mom-to-be bent on keeping up your workout routine, the trick is to consult your doctor, know your limit and have a plan for each trimester. "Pregnancy should not be a state of confinement," said Raul Artal, chairman of the department of obstetrics, gynecology and women's health at Saint Louis University School of Medicine. "Healthy pregnant women should stay active, but take into account that their bodies change during pregnancy." Artal, an author of the American College of Obstetricians and Gynecologists' guidelines on exercise during pregnancy, advises women to maintain their current level of training, whether it's biking, running or lifting. If you were squatting 125 pounds before donning maternity wear, then you can probably keep it up as elastic-waist pants take over your closet. You may have to lower the weight as the pregnancy progresses, however, if you start developing back pain. It's common for pregnant women to suffer from lordosis, a curvature of the spine that can cause lower back pain during strength training, Artal said. Proper technique is essential to prevent injury, especially at the tail-end of the pregnancy when your body will have a buildup in relaxin, a hormone that loosens ligaments for an easier delivery, said Michelle Mottola, director of the R. Samuel McLaughlin Foundation-Exercise and Pregnancy Lab at the University of Western Ontario. Joints might be prone to injury because of the higher hormone levels. So it's best to cut out any exercises that require rapid changes in direction or bouncing — no split jumps or burpees. And isometric exercise — the sorts of moves that require hold periods — is best left for post-pregnancy workouts. Stick to static moves such as squats, which are good for strengthening your abdominals and pelvic floor, the muscles and ligaments that support the womb, said Lisa Reed, a Washington-based trainer. She designs fitness and nutrition programs for each trimester of pregnancy and post-delivery. "The biggest thing with prenatal clients is strengthening the pelvic floor and abdominals," Reed said. "Abdominals are going to be vital to carrying the baby, to your posture and to the pushing stages of labor." Reed also encourages clients in the third trimester to sit on the floor with a stability ball behind their back, pushing against the ball and taking deep breaths in and out. "As you exhale and push your lower back in, you are actually using your abs to exhale," she said. "Pregnant women have to be really conscious of their breathing and remain hydrated throughout their workout." Mottola recommends that women hold off on heavy lifting, instead use lighter weights with higher counts, say 12 to 15 repetitions per set. Save the maximum reps and power lifting for after you deliver your bundle of joy to avoid putting too much pressure on your joints, Mottola said. There are some exercises that you should avoid at certain points during your pregnancy. Exercising while lying on your back is a no-no past four months, Mottola said. Your enlarged uterus could either decrease the flow of blood returning from the lower half of your body as it presses on a major vein or decrease the flow to a major artery. Reed said she advises her pregnant clients to avoid exercises such as knee lifts and high kicks that shift the pelvic floor. Anything that "puts more stress on the pelvic floor and twisting of the body is not advised in the third trimester," she said. On the other hand, swimming or any kind of exercising in the water is a great way for women to stay in shape throughout their pregnancy, Reed said. Buoyancy alleviates some of the joint stress moms-to-be experience, and lap swimming can help condition muscles. BY DANIELLE DOUGLAS, THE WASHINGTON POST  Find out which common habits could make it harder to conceive By Leah Fessler, Women’s Health You know it takes a healthy woman (and man) to make a healthy baby. But sometimes, it can be way harder to conceive than you’d like–even if it’s the right time, with the right guy, and solid health. Turns out your fertility can be affected by many more factors than you might have thought. So, if you’re trying to get pregnant, or even if you can foresee a little you sometime in the future, it’s important to learn what (often easy!) lifestyle changes might be in stock. Ready to boost your baby-making potential? Here are 17 things that can mess with your fertility: Artificial Nighttime Light We know it’s bad to stare at smartphone or tablet screens at night, but these habits can mess with more than just your sleep cycle. According to research published in the journalFertility and Sterility, artificial nighttime light exposure can harm both your ability to conceive and fetal development if you’re already pregnant. Late-night light exposure can suppress melatonin production, the “sleep hormone,” that’s also produced in the reproductive tract and blocks eggs from damaging free radicals, particularly during ovulation. Insufficient melatonin production can also disrupt a developing fetus’ internal clock, resulting in long-term problems, researchers suggest. Junk Food If you’re not consuming the right nutrients (think monounsaturated fats, zinc, vitamin D, and B6), you could be disrupting your body’s regulation of critical reproductive hormones like progesterone, insulin, and testosterone. Pick up these 5 healthy foods on your next grocery trip to boost your body’s baby-making potential. Plus, make sure you’re eating a hefty and nutritious breakfast: Research published inClinical Science found that consuming about half of your daily calories in the a.m. could increase your fertility. Your Cholesterol AND His High cholesterol won’t just harm your heart–it can also negatively impact your ability to conceive, according to a recent study in the Journal of Endocrinology and Metabolism. Researchers found that high free cholesterol in women was associated with a longer time trying to get pregnant. But get this: When both male and female partners had high cholesterol, it was even harder to get pregnant, compared to couples with normal cholesterol levels. These results held true even after adjusting for age and BMI. So, if you and your guy are hopeful for a third member, make sureboth of you check those cholesterol levels stat. Stress If you’re having a hard time getting pregnant, a spa day or yoga class could certainly be in order; a study published this year in the journal Human Reproduction found that high stress levels are associated with an increased risk of infertility. Researchers found that women with high levels of alpha-amylase (a stress hormone associated with your sympathetic nerve system) had a 29 percent lower chance of pregnancy and were two times more at risk for infertility than women with low alpha-amylase levels. No time to zip off to your favorite beach resort? Thankfully, we’ve rounded up a ton of ways to relieve stress in just five minutes or less (hint: they include chocolate!). Poor Oral Health Those pearly whites boast benefits far beyond the perfect profile picture. A study in the Journal of Periodontologyfound that women who needed fertility treatments had higher levels of gum bleeding and inflammation than those who conceived naturally. “Several studies have indicated thata woman’s oral health may be related to her reproductive success,” says Susan Karabin, D.D.S., a spokesperson for the American Academy of Periodontology. So make sure to brush, floss, and make it to your exam every six months. Smoking Hopefully, an increased risk of lung and breast cancer has made you ditch this extremely unhealthy habit. If not, perhaps this will: The American Society for Reproductive Medicine (ASRM) estimates that smoking is linked to 13 percent of infertility cases. Plus, a study in Tobacco Control found that women who were exposed to secondhand smoke six or more hours a day as adults were 36 percent more likely to have trouble conceiving. Thankfully, your fertility level will return to normal in about a year, so if you’re trying to get pregnant (or just live a longer, healthier life), cut out the cigarettes—and tell your friends and family to do the same. Your Weight In case you need another reason to hit the gym (or scale down your fitness routine if it’s extremely intensive): “Being overweight is a huge issue if you’re trying to get pregnant,” according to ob-gyn Mary Jane Minkin, M.D., clinical professor at the Yale School of Medicine. That’s because an unhealthy weight can mess with your periods and ovulation. Additionally, The American Society for Reproductive Medicine estimates that 12 percent of infertility cases are because of weight-related issues. But being underweight can be equally harmful. “Losing a significant amount of weight or excessive exercise, particularly if your BMI drops below 18 or 19, can cause lack of ovulation in extreme cases and thus affect fertility,” says ob-gyn Alyssa Dweck, M.D., coauthor of V is for Vagina. Consider this a reminder of all the amazing benefits of maintaining a healthy weight that have nothing to do with how you look. Hormonal Imbalances We know the thyroid is key to metabolism regulation, but it can also affect your ability to conceive, says Dweck. “Thyroid abnormalities may very well lead to infertility because alterations in the thyroid hormone—whether one is hyper- or hypothyroid—interfere with ovulation. Thankfully, proper use of medications and other prescribed treatments can likely correct this,” says Dweck. Read more tofind out if you could have a thyroid disorder. Medications "There are certain medications, particularly certain antidepressants and mood stabilizers, that can affect your ability to conceive by making your body produce more prolactin, a hormone that interferes with ovulation," says Minkin. So if you’re thinking about getting pregnant, talk to an ob-gyn about what medications are safe or unsafe, what might affect your ability to conceive, and which ones you’re currently taking, says Minkin. That way you may be able to find an alternative that won’t interfere with getting pregnant. Your Age Oh, the biological clock; just mentioning it makes many of us totally anxious. While many women are postponing pregnancy until later in life–whether because of their career, relationship status, or hey, they just want to (we’re busy, people!)–it’s important to realize that fertility doesn’t last forever. “Fertility for women naturally starts to decline slowly after age 32,” says Dweck. “More notably after 35 and even more pronounced after 40. Women do not produce more eggs with age, but instead are born with a finite amount. Over time, the number and quality of eggs decrease.” That said, it’s definitely possible to conceive after age 35. If you’re still seeing no success after six months of trying (compared to a year, if you’re under 35), be sure to see an ob-gyn to discuss potential complications and treatments, suggests Minkin. Breastfeeding First things first: That old wives tale about breastfeeding making it impossible to get pregnant is totally false—it’s not birth control. However, it could make it harder to get pregnant. “If you are still breastfeeding one child while going for a second it can significantly impact fertility, as high secretion of prolactin, the hormone that you make when you lactate, can interfere with ovulation,” says Minkin. Your Cervical Mucus This fluid secreted by the cervix is crucial when it comes to baby making since it helps to protect the sperm as it travels through the female reproductive tract. (Weird right? Here arenine more things you didn’t know about sperm.) Cervical mucus abnormalities may cause infertility, usually if it’s too thick, says Dweck. But luckily, this is usually treated with medication or overcome with intrauterine insemination. Another reason to quit smoking: In women, tobacco changes the cervical mucus, thus making it harder for the sperm to reach the egg, says Dweck. Lubricants Yes, they can make the process way more fun (and comfortable), but some lubes can challenge conception. “Certain lubricants can actually impair fertility by affecting sperm,” says Dweck. “If you are having issues conceiving and feeling dry during intercourse, try a sperm-friendly lubricant such as Pre-Seed, available over the counter.” Uterine Polyps or Fibroids Uterine polyps are typically small, oval or round overgrowths of endometrial tissue that remain attached to the uterine wall, and uterine fibroids are basically the same, but are composed of muscular tissue. “These benign growths may actually cause infertility,” says Dweck. “Luckily, many issues with uterine polyps or fibroids are easily correctable with surgery.” Folic Acid Deficiency If there’s one vitamin you need to be taking when you’re trying to get pregnant (and if you foresee pregnancy in the future!), it’s folic acid. Your body uses this vital B-complex vitamin to create red blood cells, and it’s crucial for expecting mothers. So how much do you need? Minkin advises up to 400 micrograms of folic acid every day. The easiest (and most reliable) way to secure this intake is by taking a daily folic acid supplement (most have 400 mcg). You can also nosh on sunflower seeds, spinach, eggs and grains like pastas and cereals for a boost. Find out if you’re getting enough folic acid. Phthalates You might be much more familiar with this baby-making threat than you think: Phthalates are a group of synthetic chemicals used in plastics and some cosmetics. According to a study presented last year at the annual meeting of the European Society of Human Reproduction and Embryology, they might compromise your ability to conceive. Previous studies have shown phthalate exposure can mess with a man’s fertility, and this study found that women with the most phthalates in their systems were twice as likely to suffer from implantation failure after IVF procedures as women with the lowest level of phthalates. Learn more about how to minimize your phthalate exposure here. Chronic Health Conditions Certain health issues, like endometriosis and diabetes, can have a significant impact on your ability to get pregnant. Read more about endometriosis and your fertility, and check out what you need to know about gestational diabetes.  If you're a mom-to-be bent on keeping up your workout routine, the trick is to consult your doctor, know your limit and have a plan for each trimester. “Pregnancy should not be a state of confinement,” said Raul Artal, chairman of the department of obstetrics, gynecology and women's health at Saint Louis University School of Medicine. “Healthy pregnant women should stay active, but take into account that their bodies change during pregnancy.” Artal, an author of the American College of Obstetricians and Gynecologists' guidelines on exercise during pregnancy, advises women to maintain their current level of training, whether it's biking, running or lifting. If you were squatting 125 pounds before donning maternity wear, then you can probably keep it up as elastic-waist pants take over your closet. You may have to lower the weight as the pregnancy progresses, however, if you start developing back pain. It's common for pregnant women to suffer from lordosis, a curvature of the spine that can cause lower back pain during strength training, Artal said. Proper technique is essential to prevent injury, especially at the tail-end of the pregnancy when your body will have a buildup in relaxin, a hormone that loosens ligaments for an easier delivery, said Michelle Mottola, director of the R. Samuel McLaughlin Foundation-Exercise and Pregnancy Lab at the University of Western Ontario. Joints might be prone to injury because of the higher hormone levels. So it's best to cut out any exercises that require rapid changes in direction or bouncing — no split jumps or burpees. And isometric exercise — the sorts of moves that require hold periods — is best left for post-pregnancy workouts. Stick to static moves such as squats, which are good for strengthening your abdominals and pelvic floor, the muscles and ligaments that support the womb, said Lisa Reed, a Washington-based trainer. She designs fitness and nutrition programs for each trimester of pregnancy and post-delivery. “The biggest thing with prenatal clients is strengthening the pelvic floor and abdominals,” Reed said. “Abdominals are going to be vital to car-rying the baby, to your posture and to the pushing stages of labor.” Reed also encourages clients in the third trimester to sit on the floor with a stability ball behind their back, pushing against the ball and taking deep breaths in and out. “As you exhale and push your lower back in, you are actually using your abs to exhale,” she said. “Pregnant women have to be really conscious of their breathing and remain hydrated throughout their workout.” By Danielle Douglas, Washington Post | August 24, 2014  Even in small amounts, alcohol can have negative effects on a woman’s health. In some ways, heavy drinking is a lot more risky for women than it is for men. Women who drink more than one drink per day increase their risk for motor vehicle crashes, other injuries, high blood pressure, stroke, violence, suicide, and certain types of cancer. Alcohol affects women differently than men, and not just because women are typically smaller and weigh less than men. Pound for pound, women also have less water in their bodies than men. When alcohol passes through the digestive tract, it spreads throughout the water in the body. The less water available, the more concentrated the alcohol. This means that, per drink, compared with a man, a woman’s organs, including the brain, are exposed to higher concentrations of alcohol and the toxic byproducts that are produced as the body breaks down alcohol. Risks
for more information: www.niaaa.nih.gov |
Dr. Jaspal SachdevDr.Jaspal Singh Sachdev is the Resident Consultant and Head of Unit of Obstetrics and Gynaecology at Park City Medical Centre a Ramsay Sime Darby Hospital. Archives
December 2016
Categories |

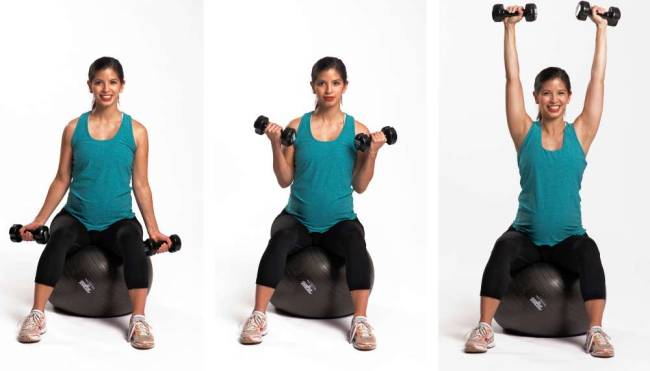

 RSS Feed
RSS Feed
