 The supermarket shelves are lined with products encouraging us to keep our lady parts clean and pleasant-smelling . Many of us still remember the line “Do you ever get that not-so-fresh feeling?” from a douche commercial years ago that made many a woman begin doubting their vaginal cleanliness at a very young age. The truth is that most women’s natural scent is normal. Your vagina doesn’t need to smell like that field of flowers on the box of feminine deodorant spray. Why does the vagina smell? The vagina is a carefully balanced ecosystem of fluid (discharge) and bacteria meant to keep the vaginal PH at a healthy 4.5. This combination of fluid and bacteria that make up the vaginal discharge that can, at times, emit certain odors. Most of these odors are natural and normal, but there are times when excess odor can signal a problem. So what is a “normal” amount of odor? After performing a very unscientific poll of all the gynecologist I know, we determined that one can smell a normal vagina from 1 foot away. More pungent odor or any associated with pain, burning or itching should prompt a visit to your provider. Some common causes of vaginal odor include: Bacterial Vaginosis (BV) – The vagina is normally colonized with healthy bacteria, but if something disturbs the ecosystem, then unhealthy bacteria like BV can take over. BV is most commonly caused by an overgrowth of the bacteria Gardnerella vaginalis. Symptoms include a thin grey, runny discharge and a strong fishy odor. The odor is more pungent when in contact with semen, so often women will first notice this as a strong odor after sex. BV is annoying and can increase your risk of other infections, but is easily treated with antibiotics. Your Diet – The old adage “You are what eat” is true, all the way down to your lady bits. Garlic, onion, asparagus, and curry are few of the more odoriferous foods known to affect body odor. Medications/ Supplements - Medications such as antibiotics can affect the bacterial balance of your vagina leading to changes in odor and discharge. Antihistamines can lead to vaginal dryness and decreased vaginal secretions, which can also have an effect. Additionally, herbal therapies and the newly popular essential oils can lead to changes in vaginal odor. Sweat - Much like your underarms, the skin around your genitals is prone to excessive sweating. Sweat when combined with discharge can escalate the natural musk to a whole new level of stank. This is a natural odor, though sometimes slightly unpleasant. To minimize the smell, change clothes after exercising and wear breathable fabrics. Hormonal Changes – The amount of discharge varies throughout menstrual cycles. Hormonal therapies, birth control pills and vaginal creams can have an effect the vaginal PH and odor as well. Menopause also leads to major changes as the decreasing estrogen levels can lead to increasing incidence of yeast infection and BV. A Forgotten Tampon – There is one odor that is so foul, it is unlike anything you have every smelled in your entire life. It’s the one smell that makes even the gynecologist gag: the forgotten tampon. The patients on many occasions have described the odors as ”it smells like something crawled up in there and died.” I would have to agree that this is an honest statement. While the odor is particularly offensive, it does resolve quickly after the tampon is removed. Rarely, the retained tampon can also lead to serious infection, so it is important to see your doctor should this occur (symptoms include a brown discharge and odor). Douching is never indicated for vaginal odor or any other reason. It only further changes the bacterial content and can spread infection. You do not need to insert anything inside your vagina to clean it: no douche, no essential oils, no soap, no Listerine (yes, these are all things I’ve had patients use to ‘clean themselves’). Simply think of the vagina as a “self-cleaning oven.” If you’re concerned about your odor, but have no other symptoms, you may first try increasing your water intake and cutting out any odorous foods. You might also take a probiotics to help restore normal bacterial balance. For proper hygiene, clean the external area of your vagina (vulva and labia) with a mild soap. If odor persists despite these measures, then follow up with your provider. By Heather Rupe, DO http://blogs.webmd.com/womens-health/2014/10/why-does-my-vagina-smell.html
0 Comments
Although breast self-exams can be life-saving, doing them every month is just one more time consuming, anxiety-provoking task on your to-do list.
Feel for lumps in the shower, then stand in front of the mirror, then lie down and feel again. Use this kind of motion, that type of pressure. Repeat every month. Kudos to you if you are making the time, but if you’re only doing them occasionally, that’s ok too. “The very rigid and structured monthly breast self-exam that you take very seriously, has kind of gone by the wayside,” said Dr. Alyssa Dweck, a board-certified obstetrician and gynecologist and co-author of “V is for Vagina.” Although major health organizations previously recommended women do breast self-exams every month without fail, studies show they don’t improve survival odds and may even increase the amount of unnecessary biopsies. Experts agree breast self-exams are a good idea but it’s more important to know what your breasts look and feel like rather than worrying too much about what method to use. “We think it’s important for women to know what’s normal for them so they would recognize a change if a change occurred,” said Susan Brown, a registered nurse and managing director of health and mission program education at Susan G. Komen. So regardless of when and how often you do a breast self-exam, here are some tips: • Do the breast self-exam when your period ends so your breasts are less likely to be tender or swollen. • Stand in front of the mirror and raise your arms above your head, then lower them at your sides. Look for any differences in your breasts. • Use the pads of your fingers to feel for lumps, bumps and tender spots. You can do it in the shower, sitting or lying down. • Use an up and down, circular or wedge (start at the outer edge of the breast and move towards the nipple and back again) motion. It doesn’t matter which one you use but do the same one each time so you know what’s normal. • Feel under your armpits for enlarged lymph nodes. Here are some changes to look for and talk to your doctor about: • Nipples that retract or are pulled in. For some women, this is normal and no reason to worry. • A lump, hard knot, or thickening in the breast or the underarm. • Dimpling or puckering of the skin anywhere in the breast. • An unusual rash or a rash that looks like an orange peel. • A sudden change in the size or shape of the breasts. It’s normal for breasts to be asymmetrical. • A clear or milky discharge from the nipple (other than breast milk). It’s not usually a sign of cancer and might be a sign of an elevated level of the hormone prolactin. Nevertheless, tell your doctor. • Spontaneous grey, black, dark green or bloody nipple discharge. • Swelling, warmth, redness, or darkening of the skin. • An itchy, scaly sore or rash on the nipple. • New pain in one spot of the breast that doesn’t subside. by Julie Revelant is a freelance writer and copywriter specializing in parenting, health, healthcare, nutrition, food and women's issues. 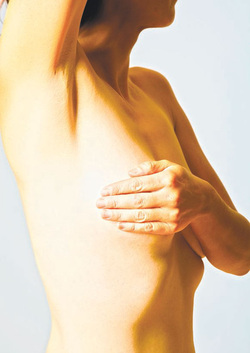 Individuals diagnosed with some form of cancer often ask themselves and their physicians, “Could I have done something to prevent this?” Women who are concerned about breast cancer also may wonder if they can prevent this potentially deadly disease, wondering if there is a pill, a vitamin, or another method to keeping the cancer at bay. Unfortunately, there is no guaranteed way to prevent breast cancer. However, there are many different steps to take that may help reduce the risk for cancer or increase the odds that if breast cancer is present, it can be found at a more treatable stage. There is no exact cause of breast cancer, but many experts agree that certain lifestyle choices as well as genetics can increase an individual’s risk. A woman’s risk also increases as she ages. When a woman is in her 30s, her risk of developing breast cancer is roughly four out of 1,000. By the time she reaches her 60s, that risk has increased to 37 out of 1,000. Though women can’t reverse the aging process, they can gain a greater understanding of additional risk factors for breast cancer and follow medical guidelines concerning breast cancer screenings. Here are some things to know: Family history: Having a sister, mother, daughter, or two or more close relatives with a history of breast cancer increases a woman’s risk, particularly if these diagnoses were made when the relatives were under the age of 50. Such women should begin testing for breast cancer at an early age. Personal history: If you’ve already experienced cancer in one breast or another part of your body, you are at an increased risk of getting cancer again. Breast cancer can turn up in the other breast or even in the same breast as before. Inheritance of genetic mutations: Individuals with mutations in the BRCA1 and BRCA2 genes are much more likely to get breast cancer, says the National Cancer Institute. The risk also increases for colon or ovarian cancer. In normal cells, BRCA1 and BRCA2 help ensure the stability of the cell’s genetic material and help prevent uncontrolled cell growth. Mutation of these genes has been linked to the development of hereditary breast and ovarian cancer. A simple blood test and a genetic work-up can point out mutations in these important genes. Race: Although Caucasian women are more likely to get breast cancer than black, Hispanic, or Asian women, black women typically are more susceptible to an aggressive type of breast cancer called basal-like tumor. Limited access to healthcare can also increase the risk of cancer fatality regardless of race. Childbearing age: Women who first gave birth after age 30 have a greater chance of developing breast cancer than women who had children before reaching 30 years of age. Women who have never had children are also at a higher risk. Women who breastfeed lower their risk for breast cancer. Hormones: Women with a longer span of “high-estrogen years” are more at risk for breast cancer. This includes women who had their first menstrual cycle prior to age 12 and women who still were experiencing menopause after age 55. Anyone undergoing hormone-replacement therapy or participating in estrogen-raising therapies also has a higher risk of developing breast cancer. While many of these factors are out of your control, there are other risk factors that you can control: Alcohol consumption: Avoiding or limiting alcohol consumption can lower your risk for breast cancer. Drinking alcohol has been traced to higher estrogen levels in the body. Obesity: Being overweight can also increase risk of developing breast cancer. Inactivity: Failure to exercise can increase your risk. That’s because regular exercise and a healthy diet contribute to the body’s defense system, ensuring it is more capable of fending off disease. Tobacco products: Use of cigarettes, cigars, or chewing tobacco increases your risk for many different cancers. Infrequent doctor visits: Routine physical check-ups by a general doctor or one who specializes in women’s health can make the difference between an early breast cancer diagnosis, for which treatment is highly successful, or late-stage diagnosis, which is not as easily treated. Those who do not go for screenings put themselves at an elevated risk. Breast cancer cannot be prevented, but there are many methods to reducing risk factors associated with the disease. Article from : http://www.downtownexpress.com/2014/10/03/breast-cancer-risk-factors/ |
Dr. Jaspal SachdevDr.Jaspal Singh Sachdev is the Resident Consultant and Head of Unit of Obstetrics and Gynaecology at Park City Medical Centre a Ramsay Sime Darby Hospital. Archives
December 2016
Categories |


 RSS Feed
RSS Feed
